What is Scleroderma?
Scleroderma is an autoimmune disorder that affects the skin and connective tissues of the body. The condition affects women more frequently than men and usually occurs between the ages of 30 and 50. The disorder causes an overproduction of collagen, which causes the skin and connective tissues to thicken, harden, and tighten. Scleroderma also causes scarring and inflammation and may lead to hardening of the blood vessels and organs. The most severe form of scleroderma is called Progressive Systemic Sclerosis.
Scleroderma Symptoms
Symptoms of scleroderma can include:
- Red, hardened, or thickened patches of skin
- Tightened skin that may restrict movement
- Skin sores and ulcers
- Skin rashes
- Swelling and pain in the joints
- Extreme responses to cold temperatures
- Digestive disorders such as indigestion and acid reflux
- Shortness of breath
- Extreme fatigue
Scleroderma Treatments
Scleroderma has no cure, and treatments target painful symptoms. Current treatments include self-care, such as moisturizers, and medical care, including steroids and physical therapy.
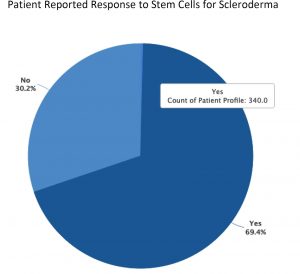
For patients with scleroderma, Innovations Medical deploys stem cells through IV along with injections. Damaged tissue attracts stem cells through growth factor chemical messages, and deployed stem cells find the damaged or diseased tissue and begin repairs. See our blogs What are Stem Cells? and Understanding Adipose-Derived Stem Cells. Innovations Medical is part of the Cell Surgical Network that has been collecting data on stem cells for scleroderma for several years. Almost 70% of scleroderma patients see improvement.
Pulmonary fibrosis is a common complication of scleroderma and stem cells work well for pulmonary fibrosis as well. Remember, most of the scleroderma and pulmonary fibrosis patients have tried many other therapies before turning to stem cells.
Cost of Stem Cell Treatments
The cost of the initial treatment ranges from $5,000 to $10,000. The range in cost is dependent on the complexity of delivering the cells back to you. For example, spine conditions require multiple physicians to deliver the cells back to your body and this requires an increase in cost as multiple doctors are involved in the procedure. For many people, the initial treatment is all that is needed; however, for some conditions, subsequent treatments may be required, and these are done at a reduced fee. Patients begin seeing results in the first few weeks of treatment. Some patients may require additional deployment.
Innovations Medical provides Stem Cell Therapy procedures at both our Dallas and Fort Worth practice locations.

