Stem Cells for Chronic Obstructive Pulmonary Disease (COPD)
The most common question asked about stem cells for COPD is: “Will they help my shortness of breath?”. There is a great deal of current research being done to answer that question and others. Many different techniques and approaches are being investigated. We want to concentrate on questions being asked by our patients. Some of the most common questions for stem cells used for COPD are:
Answer: Most of the time. Studies show improvement in most patients. Although some improvement can be quick, it appears that most improvement is slow and gradual. Our experience at Innovations Medical has
Answer: Likely. Several studies have shown improvement in lung function measurements. As mentioned above, these improvements are often slow, taking months.
Answer: Yes. Studies show stem cells are very safe when used for COPD.
Answer: One may be enough, but many patients respond better to repeated treatments over time.
Studies have attracted great interest for lung disease because current therapies treat symptoms and cannot repair lung function. Studies show stem cells are safe and the majority of studies show they are effective. Unfortunately, most studies are very small. In addition, MANY different approaches are being used, making it impossible to know the best way to use stem cells for lung disease. It may be several years before large studies develop standards for the use of stem cells. Some people with lung disease cannot wait those years, so safe treatments that can help may be the best alternative. Our experience at Innovations Medical, as part of the Cell Surgical Network, has shown our process to be safe. In a small number of patients, we have seen about a 0.5 percent increase in lung function every month. While that is a small improvement, most patients with COPD lose about 1% per month. That means that stem cell therapy is stopping worsening and slowly improving lung function.
What is Chronic Obstructive Lung Disease (COPD)?
Chronic Obstructive Lung Disease (COPD) is a debilitating lung condition that leaves patients unable to breathe or enjoy life. It is also known as emphysema, chronic bronchitis, and chronic obstructive asthma. COPD is rated as the third leading killer in the United States, killing approximately 120,000 individuals a year. Persons suffering from COPD also experience chronic disability and often low quality of life. Sufferers also require a large amount of medical care with its expense and the need to stay near medical facilities and personnel. COPD is a very limiting and deadly disease. See our blog about COPD.
This is designed to help readers gain a greater understanding of the use of adult stem cells for COPD and offer a framework for evaluating if stem cell treatment is a potential step for you or your loved one. We will cover the following:
- What are the current medical treatment options for COPD?
- Who should consider adult stem cell therapy for COPD?
- How are adult stem cells deployed for COPD?
- What results can I expect from adult stem cells for COPD?
- What to expect after your deployment?
Feel free to skip to sections that provide information that is helpful to you. For more information including definitions and descriptions of COPD visit:
https://www.lung.org/lung-health-diseases/lung-disease-lookup/copd
https://www.mayoclinic.org/diseases-conditions/copd/symptoms-causes/syc-20353679
Frequently Asked Questions
A: COPD is a chronic condition and therefore typically requires long term medications. The commonly used treatment options are:
- Inhaled medications:
- Short-acting bronco dilating inhalers which include:
- Long-acting bronco dilating inhalers which include:
- Inhaled steroids (glucocorticoids) like fluticasone. Most experts recommend that inhaled steroids only be used with bronco dilators.
- Combinations of the above inhalers
- Oral medications such as theophylline and roflumilast
- Glucocorticoids (steroids) orally, intramuscularly, and/or intravenously.
- Pulmonary rehabilitation – exercise, physical therapy, and occupational therapy
- Smoking cessation
- Oxygen therapy
- Non-invasive positive pressure ventilation
- Hospitalization is frequently required for exacerbations (worsenings)
- Lung reduction or transplant surgery
With the exception of surgery, these treatment options are all considered supportive. They help the symptoms but do not change the underlying disease. A simplified diagram of these treatments is:
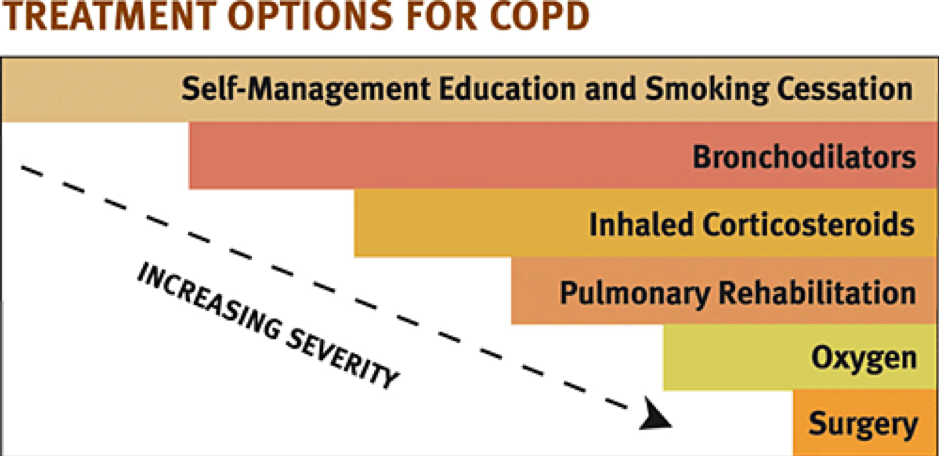
A COPD patient may be prescribed one, several, or all of these at one time or another during the course of their illness. Some patients suffer without using any treatments. The effectiveness of treatment varies greatly both between patients and over the course of the illness. Many patients with COPD do very well for many years with exercise with or without medications.
For more information on the treatment of COPD see:
https://www.lung.org/lung-health-diseases/lung-disease-lookup/copd/living-with-copd
https://www.ahrq.gov/gam/index.html
If you are doing well using these options, now might not be the right time to consider adult stem cell treatment.
A: If you are doing well with your current medical therapy, you may not be an ideal candidate for adult stem cell therapy. Persons should consider adult stem cell therapy for COPD include:
- Persons who have not responded very well to their medical treatment
- Persons who responded earlier to treatment but are no longer responding
- Persons who cannot tolerate the recommended treatment
- Persons wishing to avoid the recommended treatment such as surgery
- Persons for whom nothing has been effective.
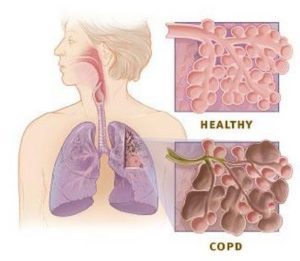
Lung changes in COPD
Adult stem cell therapy DOES NOT assure a response in these patients. However, it does offer an alternative that they may wish to consider. See our blog: Understanding Adipose-Derived Stem Cells. We will discuss the results below.
A: We refer to the process of actually using adult stem cells. For more information see our blogs What are Stem Cells? and Understanding Adipose-Derived Stem Cells. The typical deployment for COPD is intravenous. We also nebulize a small amount of the same cells and have the patient inhale it.
The IV is started in the office and the stem cells are injected into a small IV bag. This is then given to the patient over 20-30 minutes. The nebulizer is given while the IV is running. When the nebulizer and IV are finished, the IV is discontinued and the patient is discharged.
A: Although research is in progress, there are currently no treatment groups large enough to answer this question conclusively. It is important to be aware that the Food and Drug Administration (FDA) has NOT approved the use of adult stem cells for any disorder including COPD. Patients can see some improvement in a few days, but for others, nothing is seen for a few months. Those who have a cough as a prominent symptom often see improvement in their cough early on. For others, the improvement is more gradual. An early review of data has shown a slow change in the course of COPD. The primary measurement used for the severity is how much air the patient can exhale in 1 second. This measurement is called FEV1. The average COPD patient loses 1% of his/her FEV1 per month from the time of diagnosis until death. After stem cells, patients, on average, gain about ½% per month. This is a slow improvement, but over time becomes significant. The number of patients remains small but the trend is encouraging.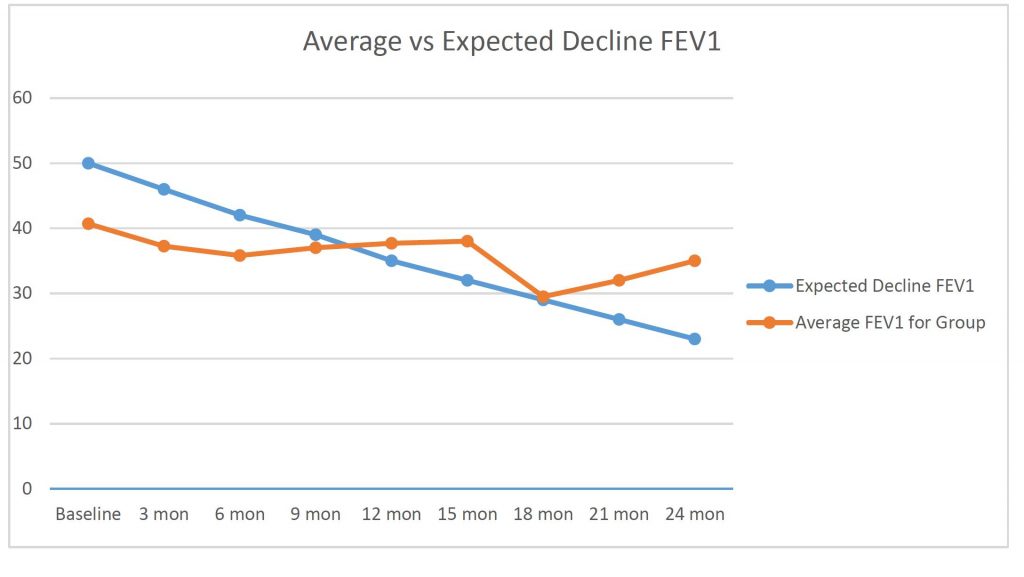 In addition, the Cell Surgical Network has collected data from a larger number of patients. In the Cell Surgical database, over two-thirds of 668 patients reported improvement in their COPD after stem cell therapy.
In addition, the Cell Surgical Network has collected data from a larger number of patients. In the Cell Surgical database, over two-thirds of 668 patients reported improvement in their COPD after stem cell therapy.
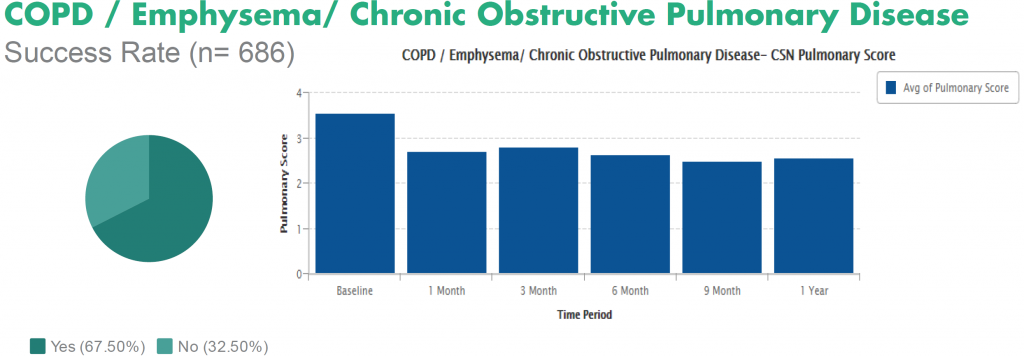 So there is increasing scientific evidence that stem cells from fat can give improvement to patients suffering from COPD.
So there is increasing scientific evidence that stem cells from fat can give improvement to patients suffering from COPD.
A: Most of the time, repeat deployment is done after the patient has seen some improvement and more improvement is sought. Occasionally, repeat deployment is done because the patient has lost some previously seen improvement. The question of how many deployments are best and how often they are needed is an area of intense interest and study at this time. It is too early to say conclusively that adult stem cell treatment promotes the growth of new lung cells.
COPD Stem Cell Treatment Cost
If you’ve been diagnosed with COPD, you might be wondering what the treatments are going to be and how much it will cost. While there are many treatments out there, one that you may or may not have heard of is stem cell treatment.
There are various medical uses for stem cell therapy and since COPD is one of them, you might find that your breathing gets easier with each treatment. Your insurance may even cover some of the $5,000 to $10,000 cost.
Ask your doctor if stem cell therapy is right for you so that you can get on the road to recovery quicker.
If You Have COPD, Innovations Medical Can Help You
Innovations Medical offers stem cell procedures for COPD at both our Dallas and Fort Worth practice locations. We hope we have answered the majority of your questions. If you have others or wish to schedule a consultation please call (214) 643-8665 or contact us online.
